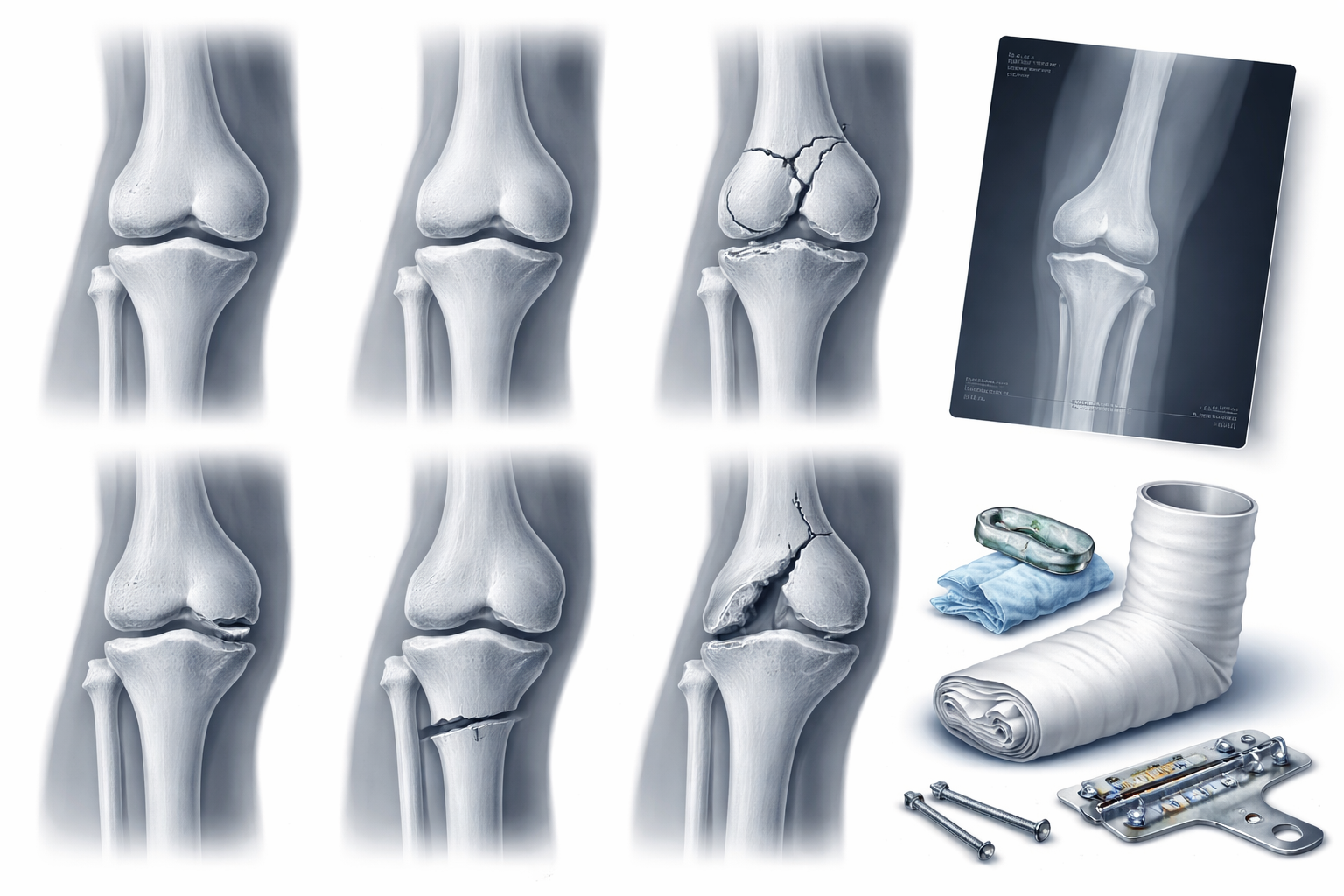
Common Fracture Types and Effective Post Fracture Recovery with Home Physiotherapy
A fracture is a break or crack in a bone that can affect movement and daily life. Different bone fracture types need different care, and recovery depends on proper treatment and rehabilitation. With the right support, including home physiotherapy, healing can become faster and safer while reducing long term complications. Read on to learn about the types of fractures, treatment options, and how proper care can support a smooth recovery.
What Happens When a Bone Breaks
A bone break can happen suddenly or develop over time due to stress or weakness. The body reacts quickly to repair the damage, but proper care is needed to avoid complications.
How Bone Fracturing Occurs
Bone fracturing happens when the force applied to a bone is stronger than the bone itself. This can happen due to accidents, falls, or repeated stress on a specific area. Sudden trauma such as road accidents or falls is one of the most common reasons. Sports injuries also put strong pressure on joints and bones, leading to fractures. Weak bones due to aging or conditions like osteoporosis increase the risk even with minor impact. Repeated strain over time can also lead to stress fractures. The severity of bone break types depends on the force of impact and the condition of the bone.
Early Signs of a Bone Break
When a bone breaks, the body gives clear signals that should not be ignored. Early identification helps in faster treatment and reduces complications. Pain is usually the first sign, often sharp and intense at the injury site. Swelling and bruising may appear within a short time. Movement becomes difficult or painful, especially in the affected area. In severe bone fracture types, deformity may be visible. Tenderness when touched is also a common symptom. Ignoring these signs can delay treatment and make recovery slower and more difficult.
Common Bone Fracture Types You Should Know
Different fracture types require different treatment approaches. Knowing the basic types of bone fractures helps in identifying the seriousness of the injury and seeking proper care.
Greenstick Fracture
A greenstick fracture is common in children because their bones are softer and more flexible. Instead of breaking completely, the bone bends and cracks partially. This type of bone fracturing usually occurs during falls or minor injuries. Even though it may seem less serious, proper treatment is important to ensure correct healing and prevent long term deformity.
Comminuted Fracture
A comminuted fracture is a severe type of bone break where the bone breaks into multiple pieces. It usually happens due to high impact injuries such as road accidents. This type of fracture often requires surgery and takes a longer time to heal. There is also a higher risk of complications because the bone is fragmented. Close medical supervision and structured rehabilitation are necessary for proper recovery.
Simple Fracture
A simple fracture is a clean break where the bone does not pierce the skin. It is also known as a closed fracture. The bone remains inside the skin and is usually treated with casting or splinting. The risk of infection is lower compared to open fractures. However, proper immobilization is important to allow correct healing.
Compound Fracture
A compound fracture is a serious type of bone fracture where the broken bone comes through the skin. This increases the risk of infection and requires immediate medical attention. Surgery is often needed to fix the bone, and antibiotics are used to prevent infection. This condition is considered an emergency and should be treated without delay.
Hairline Fracture
A hairline fracture is a small crack in the bone that may not be easily visible in early stages. It is often caused by repeated stress on the bone. Pain may start mild but can increase over time if ignored. Rest and limiting physical activity are important for recovery.
Stress Fracture
A stress fracture develops gradually due to repeated pressure on a bone. It is commonly seen in athletes and people who perform repetitive physical activities. It often affects the feet and lower legs. Early diagnosis and proper rest are important to prevent the condition from worsening into a complete bone fracture.
How Fractures Are Diagnosed and Treated
Accurate diagnosis is essential for choosing the right treatment. Medical professionals use imaging and physical examination to identify the fracture type and severity.
Diagnosis Methods
Doctors use several methods to confirm bone fracture types and assess the extent of damage. X rays are commonly used to detect most fractures. MRI scans help identify soft tissue damage and fractures that are not clearly visible. CT scans are used for complex cases such as comminuted fractures. These diagnostic methods help doctors plan the correct treatment approach.
Treatment Approaches
Treatment depends on the type of fracture and its severity. The main goal is to stabilize the bone and allow it to heal properly. Casting or splinting is used to keep the bone in the correct position. Surgery may be required for severe fractures or when the bone is broken into multiple pieces. Pain management is done using medications to reduce discomfort. Physiotherapy is introduced to restore movement and strength after initial healing. Early treatment reduces the risk of complications and improves recovery outcomes.
Stages of Bone Healing
Bone healing is a natural process that occurs in phases. Each stage plays an important role in restoring strength and function.
Inflammatory Phase
This phase begins immediately after bone fracturing and lasts for a few days. Blood collects around the fracture site and forms a clot. The body starts repairing damaged tissue and reduces inflammation. This phase prepares the area for new bone formation.
Repair Phase
During the repair phase, the body creates a soft callus around the fractured bone. Over time, this soft callus becomes a hard callus. New bone tissue starts developing and the fracture begins to stabilize. Pain gradually reduces as healing progresses. This stage is important for rebuilding the structure of the bone.
Remodeling Phase
The remodeling phase is the final stage of healing where the bone reshapes and regains its strength. The bone becomes stronger over time and returns close to its original shape. Full function is gradually restored. This phase may take several months depending on the type and severity of the fracture.
Recovery Timeline After a Fracture
Recovery time varies depending on the type of fracture and the overall health of the person. With proper care and physiotherapy, healing can become faster and more effective. Minor fractures usually heal within 4 to 6 weeks, while moderate fractures may take around 6 to 12 weeks. Severe fractures can require several months for full recovery. Physiotherapy plays an important role in improving mobility, reducing stiffness, and supporting overall rehabilitation, and home physiotherapy options are available for added convenience.
Why Physiotherapy Is Essential After a Fracture
Physiotherapy plays an important role in restoring function after bone fracture types. Without proper rehabilitation, stiffness and weakness may continue even after the bone heals.
Prevents Joint Stiffness
Physiotherapy helps maintain joint movement and prevents stiffness after long periods of immobilization. It ensures that joints remain flexible and functional.
Restores Muscle Strength
Muscles weaken when they are not used during recovery. Physiotherapy includes exercises that help rebuild muscle strength and support the bone.
Improves Mobility and Flexibility
Physiotherapy helps patients regain movement and return to daily activities safely. It improves range of motion, coordination, and overall flexibility.
Reduces Pain and Swelling
Therapeutic techniques used in physiotherapy help reduce pain and swelling. This makes the recovery process more comfortable and manageable.
Benefits of Home Physiotherapy for Fracture Recovery
Home physiotherapy offers a practical solution for people recovering from bone fractures. It allows patients to receive care in a comfortable environment.
Personalized Care at Home
Treatment is planned according to the patient condition and stage of recovery. This improves the effectiveness of therapy.
Faster Recovery with Consistency
Regular sessions at home help maintain consistency, which is important for recovery. It also removes the difficulty of traveling for treatment.
Ideal for Elderly and Post Surgery Patients
Home physiotherapy is especially useful for elderly patients and those recovering after surgery. It reduces physical strain and improves comfort.
Reduces Hospital Visits
Patients can avoid frequent hospital visits, reducing fatigue and the risk of infection. This makes the recovery process safer and more convenient.
Exercises Used in Fracture Rehabilitation
Exercises are important for restoring strength and movement after a fracture. They are introduced step by step based on healing progress.
- Range of motion exercises help improve joint flexibility and movement
- Gentle stretching reduces stiffness in affected areas
- Strength training exercises rebuild muscle support
- Light resistance exercises improve muscle function
- Balance training improves coordination and stability
Posture correction helps prevent future injuries
Tips to Support Faster Bone Healing
Certain habits can improve healing and strengthen bones during recovery.
- Eat foods rich in calcium such as milk and leafy vegetables
- Get enough vitamin D through sunlight or supplements
- Avoid smoking and alcohol as they slow down healing
- Follow medical advice carefully
- Perform physiotherapy exercises regularly
When to Seek Immediate Medical Attention
Certain symptoms after a fracture can signal serious complications and should never be ignored. Severe or worsening pain that does not improve with rest or prescribed medication may indicate improper alignment or internal damage. Numbness, tingling, or a loss of sensation can suggest nerve involvement or restricted blood flow, which requires urgent evaluation. If the bone becomes visible through the skin, it is an open fracture and needs immediate emergency care to prevent infection. Excessive swelling, redness, warmth, or increasing pain around the area may point to infection or inflammation. Additionally, if there is no noticeable improvement in pain, movement, or healing over time, it could indicate delayed healing or complications that need medical attention.
FAQs
What is the most common type of fracture
Greenstick and simple fractures are commonly seen, especially in children and minor injuries. They usually heal well with proper care and early treatment.
How long does a fracture take to heal
Most fractures heal within six to twelve weeks. Complete recovery, including strength and mobility, may take longer depending on age, health, and fracture severity.
Can bones heal without treatment
Bones may heal naturally, but improper healing can cause deformity, pain, and reduced movement. Medical care ensures correct alignment and faster recovery.
Is physiotherapy necessary after fracture
Physiotherapy helps restore strength, flexibility, and movement. Without it, stiffness and weakness may remain even after the bone has healed.
What foods help in bone healing
Calcium rich foods, protein, vitamin D, and magnesium support bone healing. A balanced diet improves recovery and strengthens bones.
Is home physiotherapy safe
Home physiotherapy is safe when done by trained professionals. It provides personalized care, comfort, and consistent recovery support without hospital visits.
Trusted Home Physiotherapy at Home in Dubai
Eureka Home Healthcare offers reliable home physiotherapy services for patients of all ages. DHA licensed and experienced professionals provide safe, compassionate, and professional care in the comfort of home. The focus is on affordable and high quality service, helping patients recover without the stress of hospital visits. Families can feel confident knowing their loved ones receive proper medical attention and support in a familiar environment.









